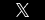
What is sciatica?
Sciatica is pain that runs down the back of the leg. It is named after the sciatic nerve, a nerve that originates in the lower lumbar spine and then travels down the back of both legs. Sciatica pain is felt all along this nerve, from the lower back, to the pelvis, hips, and buttock, and to the thighs.
What causes sciatica?
Car accidents commonly cause nerve damage because the sudden stop or change in direction causes injuries to the spine, usually a herniated disc. Other causes of sciatica include spinal stenosis, piriformis syndrome, osteoarthritis, spondylosis, and spondylolisthesis. But, as our lawyers often see, these injuries can be exacerbated by a car accident.
Herniated Discs
A disc herniation, also known as a slipped disc or bulging disc, is a common car accident injury.What is a herniated disc?
The spine is a column of bones called vertebrae. These bones provide structural support and protect the spinal cord. Spinal nerves branch out from the spinal cord, providing sensation and function to the rest of the body. In between the vertebrae are spinal discs, also known as intervertebral discs.
Degenerative Disc Disease and Spinal Stenosis
As we age, our spines suffer some wear and tear. Car accidents can cause deterioration due to the wear and tear of age to suddenly worsen and cause symptoms that were not there before. Lawyers call this aggravation of a preexisting condition. Degenerative disc disease is the term used to describe the effect that aging has on the spinal discs. Over time, the discs both dry out and crack, weakening their ability to cushion the spine against everyday movements and traumatic events like car crashes, potentially resulting in a herniated disc. Another symptom of degenerative disc disease and aging is spinal stenosis. Stenosis is the narrowing of the spinal canal, the hollow part of the vertebrae that houses the spinal cord. How does this happen? As the spinal discs weaken, the body attempts to strengthen and stabilize the spine by growing tough ligaments. These thickened ligaments in turn grow bone spurs. Both the thick ligaments and the new bony growths protrude into the space in the spinal canal, potentially putting pressure on spinal nerves and causing symptoms like sciatica.Spondylolysis and Spondylolisthesis
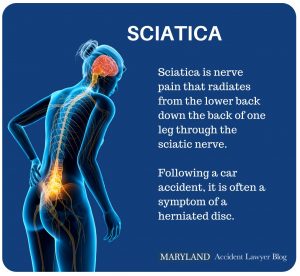
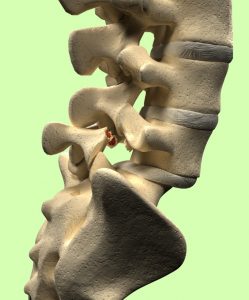 Spondylolysis is a term used to describe a stress fracture in one of the vertebrae of the lower back. Specifically, this term refers to a stress fracture in the pars interarticularis, the weakest part of the vertebrae. When the stress fracture causes the vertebra to slip out of place, this condition and its symptoms are called spondylolisthesis. The further the vertebra slips forward, the worse pain the person will generally feel, and the worse the damage will probably be to the nerves. While herniated discs can occur even in low-speed car accidents, fractures typically happen in more forceful, higher speed car accidents.
Spondylolysis is a term used to describe a stress fracture in one of the vertebrae of the lower back. Specifically, this term refers to a stress fracture in the pars interarticularis, the weakest part of the vertebrae. When the stress fracture causes the vertebra to slip out of place, this condition and its symptoms are called spondylolisthesis. The further the vertebra slips forward, the worse pain the person will generally feel, and the worse the damage will probably be to the nerves. While herniated discs can occur even in low-speed car accidents, fractures typically happen in more forceful, higher speed car accidents. How is sciatica treated?
Most of the conditions described above that cause sciatica can be treated conservatively in mild cases. This means that the symptoms can be greatly reduced or cured with a combination of physical therapy, medications, and epidural injections.
What else might be causing my pelvic and leg pain?
Sciatica is caused by the pinching of the spinal nerves. Some other conditions feel similar to sciatica but have a different origin.
What Is the Annual Incidence Rate of Discogenic Sciatica?
The annual incidence of discogenic sciatica in the United States is .5%.
How Do Disc Herniations Cause Sciatica?
Disc herniation may cause sciatica by compressing the nerve roots. The pain runs down the nerve root which is why patients often describe shooting pain.
What Is the Difference Between Sciatica and Spinal Stenosis?
Sciatica is pain caused by the irritation or compression of the sciatic nerve. Again, this is why you see shooting pain because the contact with the sciatic nerve travels down nerve roots. Spinal stenosis is the narrowing of the spinal column. This causes the vertebrae to compress the spinal nerve. Both conditions cause a nerve injury that can travel down spine.
Recent sciatica medical studies
Surgery versus Conservative Care for Persistent Sciatica Lasting 4 to 12 Months by Chris Bailey et al., New England Journal of Medicine, March 2020. Some sciatica is acute—it begins when the back injury occurs and stops soon after. Other sciatica lasts for multiple months. Researchers in this study wanted to know what treatment works best in patients with chronic pain. They screened 790 patients with a lumbar disc herniation and sciatica lasting 4-12 months. They found that surgery, specifically a microdiscectomy, was the most effective treatment. Lumbar high-intensity zones on MRI: imaging biomarkers for severe, prolonged low back pain and sciatica in a population-based cohort by Masatoshi Teraguchi et al., The Spine Journal, March 2020. MRI is a type of imaging that is used to locate the source of sciatica and guide how it can be treated. High-intensity zones show up as bright white on the scan, and their significance is debated. The researchers in this study found that high-intensity zones on MRIs are linked to longer-lasting sciatica pain. Diagnosis and treatment of sciatica by Rikke Jensen et al., BMJ, Nov. 2019. This is an overview of practice guidelines for the diagnosis and treatment of sciatica from top researchers in the field. The main points are, first, that sciatica is a symptom of several conditions. It is characterized by pain radiating down one leg. Surgery is not necessary for most patients, for whom physical therapy, exercise, and pain management helps with symptoms until the condition improves. To diagnose sciatica, imaging is only needed if the patient asks for it, if the symptoms persist for longer than 12 weeks, or if they worsen. Urinary retention and decreased anal sphincter tone are signs of cauda equina, an emergency situation. Surgery can be used to speed up recovery in patients who not improve after 6-8 weeks. A new study found that the evidence is weak that discectomy is more effective than non-surgical treatments or epidural steroid injections in reducing leg pain and disability in individuals with sciatica who are considered surgical candidates. But for those whose need for immediate relief from leg pain or disability is greater than the potential costs and risks, discectomy could be an early treatment option.Sciatica-Related Verdicts and Settlements
$616,549 – Verdict (Oregon 2023): The plaintiff claimed to suffer L3-4 disc bulging, L2-3 disc extrusion, central disc protrusion at C3-4, compression of nerve roots at C4 and C7, cervical/thoracic radiculopathy, lumbar spondylolisthesis at L2-3, bilateral sciatica after being struck by a tractor-trailer at high speeds. Verdict included $80,000 in medical expenses.
$40,000 – Verdict (Maryland 2022): Plaintiff stopped at a red light when he was rear-ended by the defendant. The plaintiff allegedly suffered loss of consciousness, L5-S1 herniation with L5 radiculopathy, lumbago with right side sciatica; cervical, shoulder, and lumbar/low back sprains, spondylosis and a facial contusion.
$79,893 – Verdict (Massachusetts 2020): A man’s vehicle was rear-ended at a red light. He suffered right-sided sciatica, a right hip tear, lower back pain, a right sacroiliac joint arthropathy, and walking difficulties. The man alleged that the other driver’s negligence caused the collision and his injuries. He claimed that the other driver failed to keep an appropriate distance, failed to control his vehicle, and excessively sped. The other driver disputed the relationship between the collision and the man’s claimed injuries. A jury ruled in the plaintiff’s favor and awarded $65,000, which the court reduced to $63,000. However, prejudgment interest increased the man’s net award to $79,893.
$145,000 – Verdict (Maryland 2020): A motorist hit a woman’s vehicle and fled the scene. The woman suffered sciatica, spinal strains, and post-traumatic stress disorder. She underwent chiropractic and physical therapy. The woman sued her insurer for failing to pay her uninsured motorist benefits. The insurer contested the woman’s claims, arguing that she only suffered soft-tissue injuries and the aggravation of her pre-existing mental health issues. A Baltimore City jury awarded $145,000.
$655,693 – Verdict (Florida 2019): A municipal-owned sanitation truck hit a 28-year-old woman’s westbound vehicle at an intersection. The woman suffered sciatica, disc herniations and bulges, right knee derangement, and post-traumatic headaches. She underwent facet injections and radiofrequency ablation to her lumbar spine. Despite undergoing these treatments, she claimed permanent injuries. The woman testified that before the collision; she had no prior neck or back issues. She also alleged the sanitation truck driver’s negligence made the City of St. Petersburg vicariously liable. The city disputed the causes of the woman’s injuries, arguing that her conditions were degenerative and unrelated to the collision. A jury ruled in the woman’s favor and awarded a $655,693 verdict.
$107,000 – Verdict (Washington 2019): A 64-year-old man suffered a bulging lumbar disc with sciatica, cervical facet syndrome, and the aggravation of a right knee injury after being involved in a chain-reaction collision. He underwent epidural injections for his bulging disc and radiofrequency neurotomy for his cervical facet syndrome. Despite undergoing treatment, the man claimed seven percent bodily impairment. He alleged that the tortfeasor’s failure to safely operate his vehicle caused the collision and his injuries. A jury returned a $107,000 verdict.
$90,000 Verdict (Connecticut 2019): A man and his female passenger suffered neck injuries after their vehicle was struck head-on. The man suffered sciatica and finger and toe tingling, while the woman suffered a neck strain. They alleged that the other driver’s inattentive driving caused the collision and their injuries. The jury awarded a $90,000 verdict.
 Maryland Accident Lawyer Blog
Maryland Accident Lawyer Blog